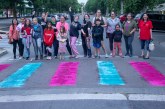Davis Vanguard’s weekly highlights from CDCR’s COVID-19 crisis
Incarcerated Narratives
Marcus Henderson is the editor-in-chief of San Quentin News, a monthly newspaper run by 15 San Quentin prisoners. He has been incarcerated since 2001 and will be eligible for parole in May 2022.
Once the pandemic broke out, Henderson knew it would only be a matter of time before the virus hit San Quentin and he was right.
San Quentin has reported over 2,200 confirmed cases and 28 deaths since May. Henderson also contracted COVID-19 during the prison’s massive outbreak.
Prison authorities shutdown the paper along with the other educational programs to limit contact between the population. However, following a six-month hiatus, the publication resumed printing in August, in part with the help of a grant from the Chan Zuckerberg Initiative.
Henderson spoke to CPJ about how he runs the newspaper and his experience living through the pandemic.
CPJ asked Henderson what it was like reporting and producing the newspaper prior to the pandemic. Henderson said, “Since we are a monthly, we would have all the scheduled events for the month (graduations, concerts or special celebrity visits) on our big white board and the staff would sign up to cover the event.”
All 15 staff members would select the front page story together and have sessions where anyone can “air out” issues and check-in with each other to make sure they are doing okay. Staff members are trained to interview people including family members.
Henderson and his team covered the first COVID-19 outbreak in San Quentin. He said that in the early days of the pandemic, the virus was contained until prisoners were transferred in from Chino at the end of May.
Henderson shares, “For most of us who have been here for years, we know that once something gets in here, it’s going to spread like wildfire…there’s no avoiding it.”
He heard rumors about inmates dying and by the time his team would finish investigating, they’d hear someone else died. He says, “You know someone really died when the guards would come and get the remainder of their property.”
During the initial outbreak, Henderson wrote about what he saw and described it as, “…alarms and things looking like a sci-fi movie that was real.” He shared, “When I tested negative for COVID-19 and my cellmate tested positive, I knew it was just a matter of time…no matter how much you wipe down, there was no way to social distance. He was right there.”
There was not enough space or areas to quarantine until the administration put tents up. When Henderson tested positive, he lost his sense of smell and experienced chest pains. He was put in a tent after he got better, but was glad to be outside.
“We didn’t stop publishing…” Even though access to the newsroom was cutoff, Henderson’s team continued reporting by writing for different outlets and building relationships with the Society of Professional Journalists.
There are tents for isolation, but there is still overcrowding with a lot of older inmates and those with underlying medical conditions.
For Henderson, “The thing about prison is once something gets in, it’s in, you can try to manage it, but just spreads fast.”
Henderson is finding ways to work and adapt to the new environment, and is happy to resume publishing. The newspaper has been able to start a fellowship program and strengthen ties with former staff who are now home.
Henderson finds comfort and solidarity in publishing for the newspaper again. It’s rewarding for him to keep the incarcerated population, even those in solitary confinement, informed about what is going on.
He goes on to say, “Our paper promotes self-help, rehabilitation, and education…We let incarcerated people, their families, and officials (prison or elected) know what is possible with change.”
“I think it helps with their mental health, that they don’t feel completely closed-off.”
CDCR Confirmed COVID-19 Cases and Outcomes
As of Jan. 8, there have been a total of 42,954 confirmed COVID-19 cases in the CDCR system – 4,791 of them emerged in the last two weeks. 14 percent of the cases are active in custody while 1.4 percent have been released while active. Roughly 84 percent of confirmed cases were resolved.
There have been 150 deaths across all facilities. 133 incarcerated persons are currently receiving medical care at outside healthcare facilities.
In the past week, 21 people died from what appear to be complications of COVID-19 at Richard J. Donovan Correctional Facility (RJD), California Medical Facility (CMF), California Health Care Facility (CHCF), California State Prison, Los Angeles County (LAC), Calipatria State Prison (CAL), Mule Creek State Prison (MCSP), Correctional Training Facility (CTF), North Kern State Prison (NKSP) and California Correctional Institution (CCI).
These are the first deaths reported at NKSP, CRC, CAL and CMF.
CDCR officials have withheld their, citing medical privacy issues.
RJD, in particular, has been experiencing a large outbreak, with nine deaths already reported.
“I want CDCR to be held accountable the negligence they’ve done. This is all them, it’s not the visitors. I want them to stop the transfers so this way the spreading will stop,” said Mary Estrada, a Prison Inmate Advocate
Estrada, whose husband is incarcerated at Donovan, says she plans to hold rallies near Donovan to bring more awareness.
CDCR released a statement in regard to the outbreak.
“RJD is following isolation and quarantine protocols per public health and health care guidance for the incarcerated population and has designated separate isolation units. Additional staffing resources are being redirected to RJD to offer immediate assistance with operations and/or health care.”
As of Jan. 3, all employees will be tested twice a week, according to the statement. If a staff member tests positive, they won’t be allowed in the prison and will have to immediately quarantine.
This week, CDCR is also beginning to offer COVID-19 saliva tests as an alternative to nasal swabs, according to corrections department emails.
The new option comes as CDCR deals with rising numbers across many of its facilities, including the California Men’s Colony (CMC) in San Luis Obispo, which has reported 865 positive cases in the last two weeks and currently has 872 active cases.
Department spokeswoman Elizabeth Gransee says that the tests are available now from MiraDX, the department’s contractor for the tests, and will be distributed to prisons across the state in the next few weeks.
The introduction of saliva tests came two weeks after Corrections Secretary Kathleen Allison told employees they would be prohibited from entering prisons and sent home without pay if they refuse a COVID-19 test.
A Dec. 30 email from Labor Relations Office Chief Candace Murch said saliva testing would start Monday at eight prisons: CSP Los Angeles County (LAC), California City Correctional Facility (CAC), Kern Valley State Prison (KVSP), Salinas Valley State Prison (SVSP), North Kern State Prison (NKSP), Mule Creek State Prison (MCSP), Substance Abuse Treatment Facility (SATF) and State Prison, Corcoran (COR) and Pleasant Valley State Prison (PVSP).
In the past two weeks, California State Prison Solano (SOL) has tested the most individuals, 81 percent of its population.
California Correctional Institution (CCI) has tested the least, just 7 percent of its population.
There are currently 95,099 incarcerated persons in California’s prisons – a reduction of 27,310 since March 2020, when the prison outbreaks first began.
Vaccine
According to CDCR, by next week all facilities would have started to vaccinate per state and federal guidelines in phase one. California Health Care Facility (CHCF) received the first shipment of vaccines on Dec. 21 and started vaccinating staff and patients in nursing housing less than 24 hours later.
Initial vaccine clinics started at CHCF, California Medical Facility (CMF) and Central California Women’s Facility (CCWF) as part of Phase 1A based on the level of care provided at these institutions. Vaccination of front line workers at other institutions followed shortly after.
San Quentin
The Prison Industry Authority (PIA) at San Quentin, which under normal circumstances serves as a site for prison labor operations, was converted into a holding area for COVID-19 patients in early July. Since then, hundreds of sick individuals have been relocated to the PIA for close medical attention and isolation from the prison’s healthy population.
A patient arriving at the PIA will find 240 cots, situated roughly 6 feet apart, each fitted with a cushion mattress, disposable sheet, two blankets, and a small pillow. During the height of San Quentin’s coronavirus outbreak, 40 nurses, paramedics, and doctors from VxL Enterprises’ Tactical Medical Services Division, a government-contracted medical provider, staffed the new quarantine unit.
Patients within the PIA have different medical needs. Some arrive in critical condition, requiring EKG monitoring, intravenous fluids, or respirators, while others are asymptomatic and are merely isolating from the at-large population.
The old factory building now home to those within San Quentin battling the deadly coronavirus has received mixed reviews from its current and former residents.
To many, life within the PIA presented an uncomfortable change of scenery. Individuals accustomed to life within a cell now bear the inconveniences of dormitory living, with a major drawback being the absence of a personal toilet. Additionally, those relocated to the PIA lost access to the prison canteen, quarterly packages, cell property, telephones and their personal televisions.
According to San Quentin News contributor David Ditto, the question “when can I go back to my cell?” was posed hundreds of times a day during the height of the pandemic in July.
“Why am I being punished?” said Marty, a San Quentin resident with an asymptomatic case of coronavirus at the PIA. “Why am I even here? I don’t have any symptoms.”
“Readjusting to the cell was rough,” said another resident speaking anonymously. “This up here sucks.”
For others, however, the PIA was a refreshing break from the months of shelter-in-place orders that restricted individuals from leaving their cells.
“I didn’t know how depressed I was until I got outta that cell,” said Lenny, who had been confined to his West Block cell for over 4 months before arriving at the PIA.
58 year-old Ronald Melville, among the first residents at the PIA, spoke highly of his experience at the unit. Melville was placed in the PIA to receive specific medical attention, and was diagnosed with COVID-related pneumonia and subsequently relocated to St. Francis Memorial Hospital where he spent 4 days in the ICU.
“I don’t know if I’d still be alive today if it wasn’t for what’s going on right here in PIA,” Melville said upon his return to San Quentin. “I can’t thank the people here enough.”
After two more weeks at the PIA, Melville was able to regain his ability to walk and talk, later echoing a similar sentiment of frustration as other incarcerated individuals who battled extreme conditions related to the deadly virus.
“I’m already serving my sentence, but this COVID feels like another sentence on top of that. I didn’t sign up for all this.”
Effect on Public
CDCR’s response to the pandemic has received a substantial amount of criticism since March, corroborated by a series of reports released by the Inspector General citing misguided and loosely enforced protocol that “increased the risk of additional, preventable infections.”
Inspector General Roy Wesley’s report identified instances where CDCR’s decisions countered the effort to reduce the presence of coronavirus in California state prisons, such as the decision to downscale mask mandates for staff and incarcerated persons as cases were rising rapidly in June.
Parts of the report suggested poor internal management at certain facilities, such as California State Prison, Los Angeles, where one staff member responded to a survey stating “the majority of custody staff refused to wear PPE and when this was reported to supervisors, their repeated response was that the mandates were unenforceable because these were adults.”
Additionally, the report found fault in screening practices throughout the CDCR’s 35 adult institutions, concluding that such directives were “vague, which appear to have caused inconsistent implementation among the prisons.”
“We believe these inconsistent practices likely contributed to some staff and visitors entering prisons without having been screened,” the report stated.
According to a survey, 5% of department staff reported not being screened on certain occasions. Between May 19 and June 26, multiple OIG investigators were able to enter prisons for inspection without receiving screening measures.
Despite widespread criticism from public and government actors, the CDCR has remained adamant that its response to the COVID-19 pandemic has been both effective and transparent.
In November, the department circulated a video to staff members warning that “mask use is not only imperative for the health of themselves and all those around them but that it’s also mandatory and those who do not comply will face disciplinary action.” However, rising case numbers at many facilities have continued to undermine the supposed efficacy of the department’s efforts.
“For most of us, everything about our daily routines has changed, including the requirements that we wear a mask at work,” said Dr. Joseph Bick, Director Division of Correction Health Care Services. “In spite of all your efforts, we continue to see COVID outbreaks in our institutions. Many of those outbreaks have been linked back to staff not consistently following our policy on the use of (PPE), such as face coverings.”
The dichotomy that exists between CDCR’s claims and case statistics has led many to conclude that a sharp increase in early releases is necessary to curb the spread of coronavirus within prisons.
“You can’t really social distance in prison,” said Alice Davis, who recently gathered outside of the Correctional Training Facility in Soledad to protest living conditions. “You live with a person in (a room) the size of a bathroom.”
Davis’ husband is currently housed at CTF, which as of the Dec. 19 protests held 880 active cases— the second-most in the CDCR system. Davis has struggled with the adapted visitation process which has barred her from seeing her husband since March. Under current protocol, individuals are allotted a free 30-minute video conference every 30 days.
“I’m very fortunate that I have a very strong support system, with my son, my family. I know I won’t see him, I won’t hear his voice,” Davis told The Californian. “This has been my life, and a lot of other families are also having a difficult time.”
CDCR Staff
There have been at least 13,494 cases of COVID-19 reported among prison staff. 11 staff members have died while 10,128 have returned to work. 3,366 cases are still active.
CDCR Comparisons – California and the US
According to the Marshall Project, California’s prisons rank second in the country for the highest number of confirmed cases, following Federal prisons. California makes up 12.6 percent of total cases among incarcerated people and 7 percent of the total deaths in prison.
California also makes up 15 percent of total cases and 8 percent of total deaths among prison staff.
Division of Juvenile Justice
As of Jan. 8, there are 61 active cases of COVID-19 among youth at the Division of Juvenile Justice facilities. 121 cases have been resolved since the first case was diagnosed in June.
References:
https://www.sanluisobispo.com/news/local/article248291580.html
https://www.themarshallproject.org/2020/05/01/a-state-by-state-look-at-coronavirus-in-prisons
https://sanquentinnews.com/pia-shifted-its-focus-to-covid-19-care/
https://sanquentinnews.com/covid-19-kills-28-san-quentin-incarcerated/
By Julietta Bisharyan, Nick Gardner and Jaskiran Soomal