
By Dorrin Akbari & Mengyu Yang
This report is written by the Covid In-Custody Project — an independent journalism project that partners with the Davis Vanguard to bring reporting on the pandemic in California’s county jails and Department of Corrections and Rehabilitation (CDCR) to the public eye. Visit our website to view and download raw data on cases, testing, releases and vaccinations.
Introduction
Following several outbreaks at the onset of the pandemic and recent vaccine rollouts for both staff and incarcerated persons, California Department of Corrections and Rehabilitation (CDCR) facilities are experiencing record low COVID-19 case numbers (1). However, the pandemic is far from over in California’s prisons. While California Correctional Health Care Services (CCHCS) has made significant progress in vaccinating the incarcerated population and prison staff members, there is still work to be done.
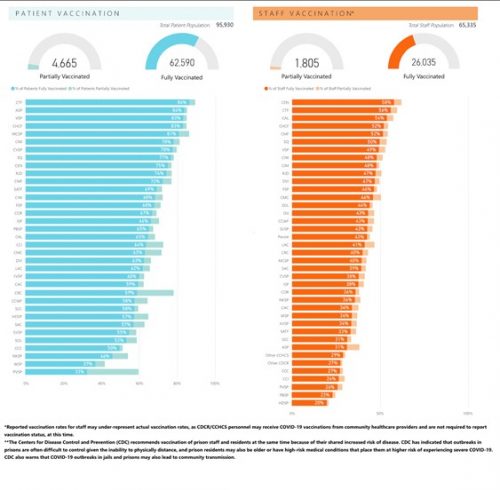
As of May 2, 2021, there have been 49,220 confirmed COVID-19 cases and 222 deaths within CDCR institutions. Of the 95,930 individuals incarcerated in CDCR facilities, 4,665 have been partially vaccinated (5 percent), and 62,590 have been fully vaccinated (65 percent).
Though the steady vaccine distribution to the incarcerated population has minimized the risk of individuals contracting COVID-19 in the dangerous congregate settings of CDCR prisons, the risk of prison staff introducing the virus into the population persists and cannot be overlooked. Staff members are the primary vector for patient infections. In previous outbreaks, infections have spread between yards or buildings of the same prison through staff movements.
Staff compliance—or lack thereof—with testing and social distancing protocols directly impact the level of risk to which incarcerated individuals are exposed.
Below is a reflection on CDCR staff behavior over the course of the pandemic with a focus on what went right, what went wrong, and what CDCR and CCHCS can do moving forward to best protect the incarcerated population.
Staff Screening and Testing
In March 2020, the CDCR took several steps to mitigate the risk of staff and visitors introducing COVID-19 into its prisons:
- March 11 — CDCR suspended normal visitation.
- March 14 — CDCR implemented verbal screenings of staff and visitors for signs and symptoms of COVID-19.
- March 27 — CDCR began temperature screenings of staff and visitors.
Following an April 2020 request by the Speaker of the California State Assembly, the Office of the Inspector General (OIG) launched an investigation into the policies, guidance, and directives the CDCR instituted in response to the COVID-19 pandemic.
The first report in the three-part OIG investigative series focused on staff screening practices such as those listed above and was published in August 2020.
Among other observations, the report concluded that inconsistent screening practices may have increased the risk of COVID-19 exposure within California’s prison system.
The OIG’s findings were based on multiple impromptu visits conducted by OIG staff at a sample of five CDCR prisons (California Health Care Facility; California Institution for Men; California Institution for Women; California State Prison, Los Angeles County; and San Quentin State Prison). Additionally, staff members from said prisons, as well as those in Avenal State Prison and Chuckawalla Valley State Prison, were surveyed to obtain another perspective on the screening process. Of the more than 12,000 staff members surveyed, 4,161 submitted responses for the OIG’s review.
Based on their direct observations, the OIG highlighted two points of failure in the CDCR’s screening process:
- Not everyone who entered prison facilities was screened.
- Malfunctioning equipment and insufficient training of staff likely diminished the effectiveness of screenings that did occur.
Failure to Screen
Due to a lack of standardized guidance from the CDCR, prisons were left to determine their screening processes on their own. Two primary methods of screening emerged: (1) funneling every vehicle to a single screening post; or (2) screening staff and visitors after they had parked their vehicles and walked to a screening area. The OIG found the latter method to be more prone to screening failures—it was the method that had been adopted by the majority of CDCR facilities.

OIG staff reported that they were not screened during 38 of their 212 prison visits at 34 of the 35 prisons statewide between May 19 and June 26, 2020. That amounted to a nearly 20 percent failure rate to screen for signs and symptoms of COVID-19.
Prison staff who participated in the OIG’s survey corroborated these findings, with 4.6 percent of respondents reporting that they had not always been screened upon entry. These rates of screening failure were further broken down between the seven institutions surveyed. San Quentin had the highest failure rate reported by respondents—7 percent.
The OIG attributed these failures to lack of visible guides to screening locations; the existence of areas beyond the facilities’ secure perimeters in which staff and incarcerated persons had the potential to interact prior to reaching a screening location; and, in some glaring instances, explicit failure to enforce or verify the administration of screenings.
Ineffective Screening
Even when CDCR facilities screened staff and visitors as required, the OIG found the effectiveness of some of those screenings may have been compromised by two factors: malfunctioning equipment and a lack of training.
70 percent of screeners surveyed by the OIG reported that their thermometers malfunctioned during staff and visitor screenings.

While the CDCR’s March 2020 memorandum implementing temperature checks stated that screeners should have a backup thermometer and additional batteries available, it made no mention of how screeners should proceed if they were unable to obtain accurate readings at all.
In fact, the OIG found that most screeners surveyed, specifically 67 percent, had received no training on their prison’s screening process, and of the few who had, none received training related to the thermometers they were issued.
Proper training should have extended beyond thermometer usage because some staff and visitors may not have been familiar with all of the common COVID-19 symptoms. Further, screener training should have included instructions on how to properly observe individuals and look for characteristic signs and symptoms.
Essentially, the CDCR’s screening directives failed to include enough specificity to ensure staff screening processes were consistently and effectively implemented across its facilities.
The lack of training and quality tools provided to the screeners, increased the risk of symptomatic and potentially infected staff entering CDCR prisons, thereby infecting the incarcerated population.
Testing: A Locus of Substantial Progress
On Dec. 21, 2020, CDCR and CCHCS issued a joint memorandum requiring that all CDCR facility employees be tested for COVID-19 on a weekly basis while working onsite. The memorandum noted that “any employee who refuses to comply with mandatory COVID-19 testing shall not be permitted to enter the institution or facility and shall be placed on approved dock (without pay) until they comply with mandatory testing.”
In a Joint Case Management Conference Statement in re Plata v. Newsom filed on Jan. 26, the attorneys for the plaintiffs described the process used by several CDCR facilities to test their staff members for COVID-19:
- Weekly, prison staff would review a list of employees who tested the week before.
- That list would be compared to the list of employees who worked that week.
- If the comparison revealed that an employee may have worked while having not been tested, the facility would investigate the case.
- If an employee was confirmed to have not been tested before working, they were not immediately placed on leave; instead, they were directed to get tested and only placed on leave if they then refused to test.
- If the comparison revealed that an employee may have worked while having not been tested, the facility would investigate the case.
Plaintiff’s counsel identified several issues with the process, which they submitted to the CDCR for review:
-
- The process only identified non compliant staff the week after they had worked without having been tested.
- The process did not identify whether particular employees were tested every 7 days, as required by the guidance, but instead checked if employees were tested at some point during the week they worked.
- For example, a staff member could be tested on the Monday of one week and the Friday of the next (11 days apart).
- Staff who called in sick or whose symptoms were discovered during entrance screening were sent home for the day but were not required to be tested or isolate at home for any period of time before returning to work.
- Staff who failed to comply with mandatory testing were given another opportunity to test rather than being placed on leave as the memorandum recommended.

Following months of back and forth between the CDCR, CCHCS, and the Prison Law Office, CCHCS and CDCR made substantial progress in addressing issues raised about staff screening and testing.
CCHCS and CDCR issued a Revised Guidance to All Staff Outlining Entrance Screening Procedures, which went into effect on March 1.
The new screening and testing procedure is as follows:
- When entering a CDCR facility, staff and visitors must submit to a series of questions and have their temperature taken.
- A question asking if the individual has been tested for COVID-19 within the last 7 days is now included as part of the screening.
- If a staff member has not been tested in the last 7 days or if they have a temperature of 100.4 degrees or more, they will immediately receive a rapid test.
- Each of the CDCR’s institutions is now equipped with rapid COVID-19 testing machines.
- CCHCS is in the process of obtaining a rapid test called BinaxNOW, which does not require a machine and can be administered more easily onsite.
- Staff who have tested within the last 7 days will be asked if they have experienced any COVID symptoms in the past 10 days or if they have been in close contact with someone with lab-confirmed COVID-like symptoms without appropriate PPE.
- If they have, they will receive a rapid test
- People who receive a positive test or have symptoms will be denied entrance to the CDCR institution for 10 days.
While there is still room for improvement in the process, namely its reliance on staff self-reporting compliance with the testing policies during entrance screening, the new procedure represents significant efforts on the part of CCHCS and CDCR to prevent staff from exposing the incarcerated population to COVID-19.
The tireless work done by the Prison Law Office and other firms and advocacy groups on behalf of incarcerated individuals directly impacted the progress made with regard to staff screening and testing. Their work continues today.
Face Covering and Physical Distancing
Per the March 2 Case Management Conference Statement in re Plata v. Newsom, all staff members are subject to corrective action as opposed to formal adverse action for noncompliance with face covering and physical distancing requirements. Employees, contractors, and visitors who fail to comply with mask-wearing protocols are subject to “progressive discipline.” The logs provided by prisons showed that almost all staff who failed to comply with the mandates, both at California State Prison, Solano, and facilities statewide, received verbal counseling or a letter of instruction.
Meanwhile, California State Prison, Solano had employed a more punitive approach to incarcerated persons who violated mask-wearing mandates by issuing immediate Rules Violation Reports (RVRs). These reports may result in an individual serving more time because RVRs often result in a loss of time credits. Further, the parole board may use RVRs to support a finding that an individual is unsuitable for release.
In response to a report published in October 2020 which identified frequent noncompliance by both staff and incarcerated persons with face covering and physical distancing requirements, Judge Jon S. Tigar invited the OIG to conduct follow-up monitoring at CDCR facilities to observe and report staff’s and incarcerated population’s compliance with the department’s current requirements.
The OIG staff conducted unannounced visits to 17 prisons and 2 juvenile facilities from February 7, 2021 to March 6, 2021. At each prison visited, the OIG staff checked multiple locations and viewed a sampling of video recordings when possible. The visits were focused on the staff’s and incarcerated persons’ compliance with face covering and physical distancing requirements.
Based on their observations, OIG staff concluded that although most adhered to the department’s requirements, there were still significant instances of noncompliance at several prisons and juvenile facilities.
The report generated by OIG (Exhibit B of the 3/24/2021 Joint CMC Statement) divided their observation into two columns: staff compliance and incarcerated persons’ compliance.
The OIG report also graded the two categories for each prison on a scale of significant non-compliance to full compliance. Remarks on whether the degree of compliance had changed from December 2020 were also noted on the OIG report.
In addition to the number of non-compliant individuals observed during the OIG staff’s visit, circumstantial factors were taken into consideration:
- Total number of individuals in the location;
- Whether staff was observed quickly correcting the incarcerated persons who were not properly wearing face coverings;
- Physical distancing among non-compliant individuals;
- Number of locations visited.
Taking all factors into consideration for staff compliance, OIG staff concluded that out of the 19 facilities they visited, nine facilities showed full compliance (meaning no individuals were observed without face coverings or improperly wearing face coverings); five facilities showed substantial compliance (meaning three or fewer individuals were observed without face coverings or improperly wearing face coverings); three facilities showed partial compliance (meaning four to ten individuals were observed without face covering or improperly wearing face coverings); and one facility showed significant non-compliance (meaning more than ten individuals were observed without face coverings or improperly wearing face coverings). Six facilities showed positive changes since December 2020; five facilities showed negative changes since December 2020; and seven facilities showed no change since December 2020. Four facilities remained fully compliant during both the December 2002 and current visit.
In terms of incarcerated population compliance, the OIG staff observed that only one facility showed full compliance; four facilities showed substantial compliance (meaning five or fewer individuals were observed without face coverings or improperly wearing face coverings); four facilities showed partial compliance (meaning six to ten individuals were observed without face covering or improperly wearing face coverings); and ten facilities showed significant non-compliance. Compared to the observations from the visit in December 2020, four facilities showed positive changes; eight facilities showed negative changes; and seven facilities showed no changes.
 For staff violations of face covering and physical distancing requirements, CDCR facilities had five forms of disciplinary action: verbal counseling, written counseling, letters of instruction, referrals for investigation or punitive action, and punitive actions.
For staff violations of face covering and physical distancing requirements, CDCR facilities had five forms of disciplinary action: verbal counseling, written counseling, letters of instruction, referrals for investigation or punitive action, and punitive actions.
No punitive actions were taken for any staff member between January 13 to February 23, 2021. 6 referrals for investigation or punitive action were given at four facilities; 59 letters of instruction were given at 15 facilities; 32 written counseling were given at 16 facilities; and 264 verbal counseling were given 31 facilities.
For incarcerated population’s violation of face covering and physical distancing requirements, the facilities had two forms of disciplinary actions: corrective counseling, and rules violation reports. From January 13 to February 23, 2021, there have been 114 rules violation reports given from 19 facilities; and 306 verbal counseling given from 16 facilities.
Vaccination

The CDCR has a three phase plan for prioritizing COVID-19 vaccines for CDCR/CCHCS staff and incarcerated persons.
Phase 1A opens to:
- All institutional staff;
- If vaccines are still available in allotment 1A, vaccines will be offered to non-institution staff who have or will have contact with incarcerated persons;
- Incarcerated persons in long-term care beds, age 65+, and high-risk medical cases.
Phase 1B has two tiers:
- Tier One opens to non-institution employees with current/potential, frequent contact with incarcerated persons.
- Tier Two opens to all incarcerated persons.
Phase 1C opens to all staff members.
A Centers for Disease Control and Prevention study recently showed a single unvaccinated staff member could infect many in a congregate living setting, even where most residents are vaccinated, and that those infections can cause death, including among the vaccinated.
What’s more, staff infections dramatically and negatively impact prison programming, including medical services. Two recent instances (Found in 4/27/2021 Joint CMC Statement) highlight the damaging repercussions of positive COVID-19 cases amongst staff for the incarcerated population:
- RJD Prison was forced to revert to a COVID “Tier One” program, which placed the maximum possible restrictions on prison programming, in response to more than three staff members reporting that they had tested positive for COVID-19. There had been no positive cases reported among the prison residents for weeks, yet they suffered the consequences.
- In California State Prison Sacramento, four positive cases among the staff members resulted in over 650 incarcerated individuals being put on quarantine status and having their healthcare and programming access disrupted.
On April 15, the CDCR and CCHCS issued a memorandum to staff regarding a supplemental-paid-sick-leave program designed to encourage more employees to accept the COVID-19 vaccine. The program permits staff to take time off to receive the vaccine, receive paid sick leave if they experience symptoms following receipt of the vaccine, and receive up to 80 hours of additional leave at their regular rate of pay.
Additionally, the California Correctional Peace Officers’ Association (“the Union”) partnered with the CDCR and CCHCS on April 21 to announce the creation of a COVID Mitigation Advocate Program. The program will require each facility to form a COVID Mitigation Team to “provide ongoing education to staff, at the peer level, on the importance of COVID compliance, the latest CDCR and CCHCS COVID-19 policies, the importance of mask-wearing and physical distancing, precautions that should be taken outside of work, testing, and the vaccination program.”
Despite these initiatives, the CDCR and CCHCS have not yet mandated staff vaccinations.
Looking Forward
At present, CCHCS and CDCR’s primary responsibilities are “to complete offering vaccination to all in CDCR, fully vaccinate those who want it, then address the high refusal rates among [incarcerated individuals] and among certain staff classifications statewide.”
On April 20, the CDCR and CCHCS published an Institutional Roadmap to Reopening (See Exhibit A in the 4/27/2021 Joint CMC Statement). The document provides a general guideline for facilities to reopen institutional programs, services, and activities while allowing hiring authorities to determine additional needs based on their unique circumstances.
The Roadmap to Reopening utilizes a multi-phased approach to reopening based on guidance from the Centers for Disease Control and Prevention (CDC) and the California Department of Public Health (CDPH) among others. Movement between the phases is partly contingent on the occurrence of COVID-19 outbreaks, which are defined as three or more related COVID inmate cases within a facility in the past 14 days.
The Phases
- Outbreak Phase (Phase 1)
- Most restrictive modifications in operations, programs, and services
- To move to Phase 2, the facility must have no inmate outbreak cases for at least 14 days.
- Modified Phase (Phase 2)
- Partial reopening and gradual easing of Phase 1 restrictions
- To move to Phase 3, the facility must have no new inmate outbreak cases for 28 days.
- New Normal Programming (Phase 3)
- Progressive reopening of programs and services
- If the facility experiences an inmate outbreak, it must revert to Phase 1 restrictions.
General Provisions for Each Phase
(A more detailed outline can be found in the Roadmap to Reopening)
- Outbreak Phase (Phase 1)
- Closed to in-person and family visiting
- Video visiting allowed
- No outside vendors
- Inmate workforce limited to essential functions
- Group activities limited to small cohorts of inmates within the same housing unit
- Congregate religious activities not permitted
- Programs to be closed: Offender Mentor Certification Program, in-person college, and InnovativeGrants Program/Arts in Corrections/Volunteer programs
- Modified Phase (Phase 2)
- Hybrid visiting model
- Family visiting not permitted
- Limited media access
- Inmate workforce to return
- Outside vendors permitted
- Education Courses may return to in-person where physical distancing can be maintained
- Indoor and outdoor congregate religious activities permitted where physical distancing can be maintained
- Resumption of routine clinical operations
- New Normal Programming (Phase 3)
- Resumption of all clinical operations
- Normal programming
- Normal visiting operations
- Family visiting to resume
- Rehabilitative programs to resume
- Contact sports with appropriate face coverings allowed
- Congregate religious activities allowed
With sights set on a return to a “new normal,” it’s important that each change be undertaken with an awareness that this pandemic is not yet over, with many staff and incarcerated persons still unvaccinated, while also acknowledging that prison programming and services are essential to the well-being of the incarcerated population.